Health
New Study Questions Long-Standing Use of Beta-Blockers for Heart Attack Survivors

Recent research has raised significant questions about the effectiveness of beta-blockers for heart attack survivors. Traditionally prescribed for over four decades, these medications are designed to regulate the impact of hormones and adrenaline on the heart and blood vessels. The findings from a new study involving over 8,500 patients could prompt a reevaluation of treatment protocols worldwide.
The study, conducted by researchers at Mount Sinai Fuster Heart Hospital and the Centro Nacional de Investigaciones Cardiovasculares (CNIC) in Spain, analyzed data from more than 100 hospitals across Spain and Italy. It randomly assigned beta-blockers to some heart attack survivors while others did not receive the medication. After a follow-up period of four years, the results indicated no significant differences in mortality rates, recurrent heart attacks, or hospitalizations for heart failure between the two groups.
Notably, the research revealed that women treated with beta-blockers experienced a greater than 2.5 percent increase in the risk of death compared to those not taking the medication. This finding is particularly concerning, as it suggests that the assumed benefits of beta-blockers may not apply uniformly across all patient demographics.
Dr. Amish Mehta, Director of Noninvasive Cardiology at AHN Jefferson Hospital, emphasized the importance of these findings. “For some patients, beta-blockers may not offer the significant clinical benefit that has been a standard assumption for the past 40 years,” he stated. “This challenges the long-standing practice of routinely prescribing beta-blockers to a large number of post-heart attack patients.”
The study advocates for a more individualized approach to post-heart attack care. Dr. Mehta noted that the research highlights a critical need for further investigation into the differing effects of beta-blockers on women, who may face unique physiological and hormonal factors that influence their response to medication.
While acknowledging the groundbreaking nature of the study, Dr. Mehta cautioned against immediately changing treatment protocols based solely on this research. He stated, “It’s still too early to completely overhaul our standard of care, particularly given the historical context and benefits for certain patient populations.” He plans to continue a prudent approach regarding the duration and necessity of beta-blocker therapy, especially for patients with uncomplicated heart attacks and preserved ejection fractions.
For patients with more complex heart conditions, including those with reduced heart function, beta-blockers remain an essential part of treatment. Dr. Mehta affirmed, “For patients with even mild damage from complicated heart attacks, the consensus remains that beta-blockers continue to be beneficial.”
The implications of the study extend beyond individual treatment. The differing results between men and women call for a deeper examination of how sex-specific factors might affect the efficacy and safety of beta-blockers. Dr. Mehta pointed out that women’s symptoms, types of coronary artery disease, and responses to stress could all impact outcomes, making it crucial to tailor treatments accordingly.
For those currently on beta-blockers following a heart attack, Dr. Mehta advised against abruptly discontinuing the medication. “At their next appointment, patients should discuss their treatment with their cardiologist,” he said. “We need to assess their specific type of heart attack, current heart function, and any other comorbidities or indications for beta-blocker use.”
As the medical community reflects on these findings, the potential for a more personalized approach to heart attack treatment is on the horizon. Dr. Mehta anticipates that discussions surrounding the discontinuation of beta-blockers will become more common for patients with uncomplicated heart attacks and preserved heart function, while maintaining the use of these medications for those with proven benefits.
Ultimately, the study underscores a vital principle in cardiology: “Time is muscle,” as Dr. Mehta articulated. Immediate medical attention for any chest discomfort or concerning symptoms is crucial to achieving positive outcomes in heart attack cases. The sooner a diagnosis is made and treatment is initiated, the better the prognosis for patients.
-

 Science4 weeks ago
Science4 weeks agoUniversity of Hawaiʻi at Mānoa Joins $25.6M AI Initiative for Disaster Monitoring
-

 Science2 months ago
Science2 months agoIROS 2025 to Showcase Cutting-Edge Robotics Innovations in China
-
 Science2 weeks ago
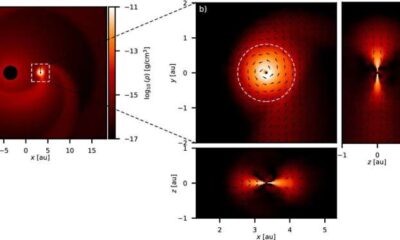
Science2 weeks agoALMA Discovers Companion Orbiting Red Giant Star π 1 Gruis
-

 Lifestyle2 months ago
Lifestyle2 months agoStone Island’s Logo Worn by Extremists Sparks Brand Dilemma
-

 Health2 months ago
Health2 months agoStartup Liberate Bio Secures $31 Million for Next-Gen Therapies
-

 World2 months ago
World2 months agoBravo Company Veterans Honored with Bronze Medals After 56 Years
-

 Lifestyle2 months ago
Lifestyle2 months agoMary Morgan Jackson Crowned Little Miss National Peanut Festival 2025
-

 Politics2 months ago
Politics2 months agoJudge Considers Dismissal of Chelsea Housing Case Citing AI Flaws
-

 Health2 months ago
Health2 months agoTop Hyaluronic Acid Serums for Radiant Skin in 2025
-

 Science2 months ago
Science2 months agoArizona State University Transforms Programming Education Approach
-

 Sports2 months ago
Sports2 months agoYamamoto’s Mastery Leads Dodgers to 5-1 Victory in NLCS Game 2
-

 Sports2 months ago
Sports2 months agoMel Kiper Jr. Reveals Top 25 Prospects for 2026 NFL Draft